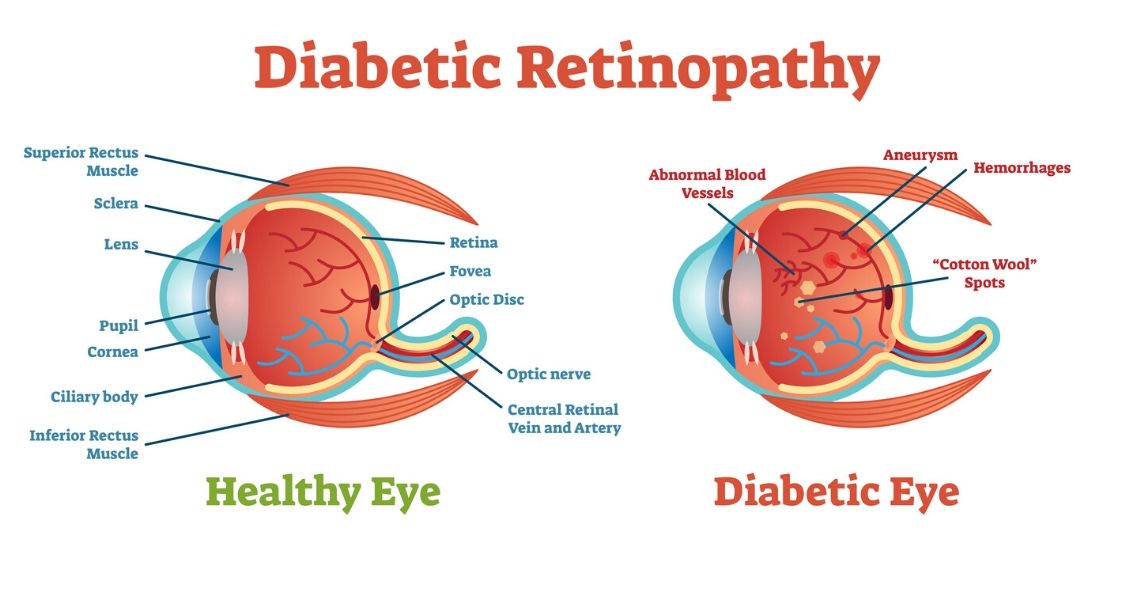
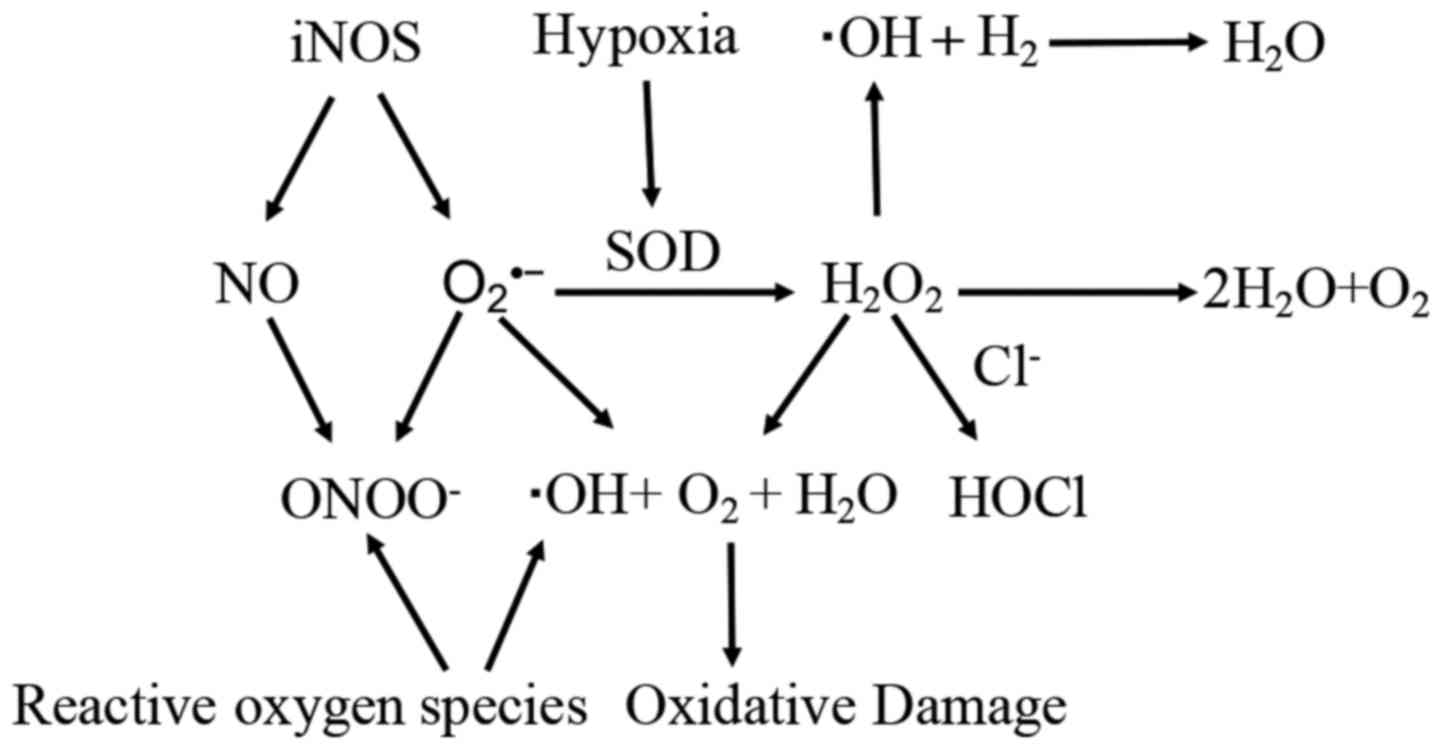
DR is the leading cause of blindness in the working force of developed countries and also acts as a significant cause of blindness in the elderly population. The overall prevalence of retinopathy among patients with diabetes is around 26%. Both clinical and experimental studies have demonstrated that DR is closely related to oxidative stress: the ROS-induced biochemical changes can induce both structural and functional abnormalities in the microvasculature of diabetic retinas, resulting in the breakdown of the blood-retinal barrier. The blood-retinal barrier is critical for partitioning the neural elements of the retina from the circulation and protecting the retina from circulating inflammatory cells and cytotoxic products. Consequently, ROS has been considered as a major contributor to the pathology of DR. In a study, it was found that HRS can suppress caspase activity, ameliorate retinal apoptosis, and reduce vascular permeability. Moreover, HRS therapy can attenuate retinal parenchyma thickening.
The ROS could upregulate the expression levels of vascular endothelial growth factor (VEGF) and enhance VEGF receptor activity via complex signaling networks. VEGF can give rise to choroidal neovascularization (CNV) in the DR and has been considered as a therapeutic target in clinical practice. Therefore, the anti-VEGF property should be considered as another functional factor for hydrogen-induced protection. Studies indicate that hydrogen might act as a valid candidate in the further clinical treatment of DR. Although the possible effect of hydrogen has not been clinically verified in DR patients hitherto, a randomized, double-blind, placebo-controlled, crossover study has already found that the supplementation of HRS improved lipid and glucose metabolism in patients with type 2 diabetes or impaired glucose tolerance. These hydrogen-induced effects might be potentially applied to diabetic complications, especially to DR, in which metabolic disorder plays a pivotal role.
Call Now: 1800-102-0908
Website: https://www.kykindia.com








 WhatsApp us
WhatsApp us