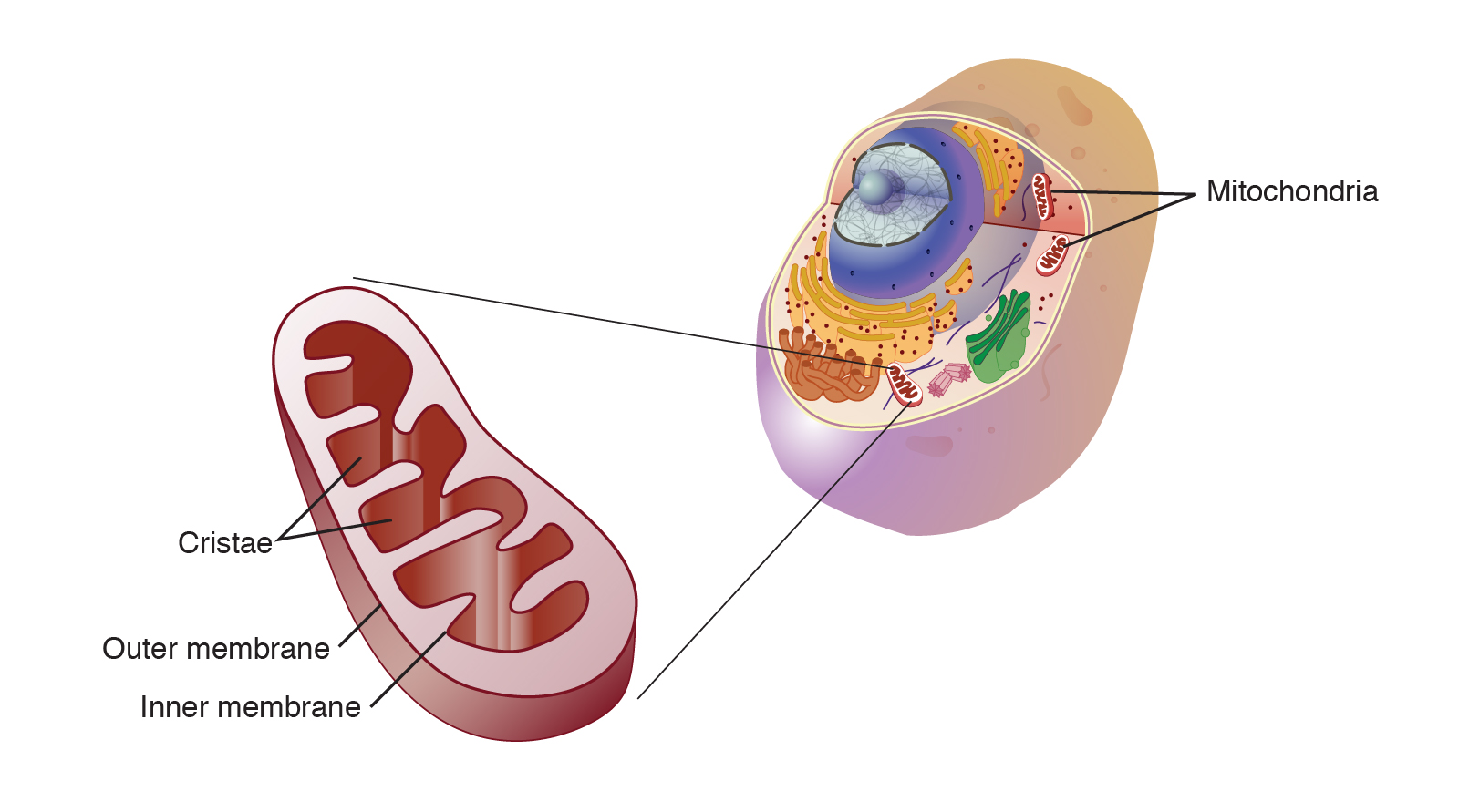
Considered as a biologically inert molecule, gaseous hydrogen (H2) has been advanced as an active member of the medical gases family, with beneficial effects of H2 become evident in various disease conditions. H2 acts as a therapeutic antioxidant that selectively reduces detrimental reactive oxygen species (ROS), and a biological messenger that mediates several signaling pathways, playing a cytoprotective role in a variety of human diseases. Due to its small size and high penetrability, H2 is suggested to be easily transported to hard-to-reach subcellular structures, including mitochondria. A preliminary study demonstrated that H2 is permeable to cell membranes and can protect mitochondria (and nuclei) from acute oxidative stress. Several trials reported favorable effects of H2 on mitochondrial function, with H2 also preserve mitochondrial membrane potential, increases adenosine triphosphate (ATP) production, and reduces swelling of the organelle.
H2 increases plasma ghrelin levels in a ß1-adrenergic receptor-dependent manner. H2 does up-regulate GHS-R1α in energy-demanding tissues rich in mitochondria (including the brain, skeletal muscle, myocardium, testis or liver) and improve markers of mitochondrial bioenergetics, it may offer a possible explanation for multifaceted energy-boosting benefits seen in H2 interventional studies that are not attributable to its antioxidant effects.
Interestingly, GLUT receptors are recognized as targets for H2 also through non-ghrelin-related mechanisms. Hydrogen treatment appears to stimulate GLUT4 translocation and glucose uptake
into mitochondria-rich tissues in streptozotocin-induced type 1 diabetic after chronic intraperitoneal and oral administration. H2 exerts metabolic effects similar to insulin through activation of AMP-activated protein kinase (AMPK) and phosphatidylinositol-3-OH kinase (PI3K). H2 effects amplify glucose uptake through both insulin-dependent (GLUT4) and insulin-independent (GLUT1) pathways. Since insulin positively affects mitochondrial bioenergetics in many energy-demanding tissues (including the skeletal muscle, brain or testis), with insulin and ghrelin network acts in interconnection, H2 could be put forward as a novel therapeutics that effectively tackles both metabolic pathways in disorders with a plausible mitochondrial dysfunction, such as diabetes mellitus or obesity.
H2 could alter mitochondrial energy metabolism by means of enhanced expression of fibroblast growth factor 21 (FGF21), a hepatic hormone that enhances fatty acid and glucose utilization. Consuming hydrogen water increases hepatic mRNA levels of FGF21, accompanied by increased oxygen consumption without influencing movement activities.
In conclusion, several alternative pathways are now advanced as main proxies for energy-modulating effects of H2, including (1) ghrelin-related upregulation of GHS-R1α; (2) ghrelin-related activation of GLUT1; (3) non-ghrelin related activation of GLUT4; and (4) non-ghrelin related enhanced expression of FGF21. Therefore, H2 may tackle other mitochondrial processes besides oxidative stress, including metabolic pathways that drive cellular energy.







 WhatsApp us
WhatsApp us